
Hadley Hooper

Audio By Carbonatix
On the last Sunday in April, Diana Lee hosted about thirty people at her hunting-lodge-themed home in Loveland. The occasion was festive, with a spiral ham, cheese fondue and a performance by a local musician.
Dressed in a pink long-sleeved shirt and gray sweat pants, Lee looked at peace in the place she had called home for the past decade-plus. As guests arrived, she showed them her bedroom, which was decorated with artificial Christmas trees and garlands.
In a few hours, she would say her last goodbyes. Lee had chosen April 28, 2019, as the day she would die.
Lee’s journey to her final day began last summer, when she learned that her breast cancer, first diagnosed in 1999, had returned. She decided that she didn’t want to go through another round of surgery, which would only have prolonged her life a little longer.
“Quality of life for me was always more important than quantity,” Lee told friends at her end-of-life celebration. So instead of waiting for the cancer to kill her, Lee took advantage of Colorado’s medical-aid-in-dying law, which voters passed in 2016.
Lee assumed her journey to the end would be relatively hassle-free.
“We thought, as boomer types, that if the law passed, all we had to do was make that choice,” Lee said. “But it’s actually pretty confusing.”
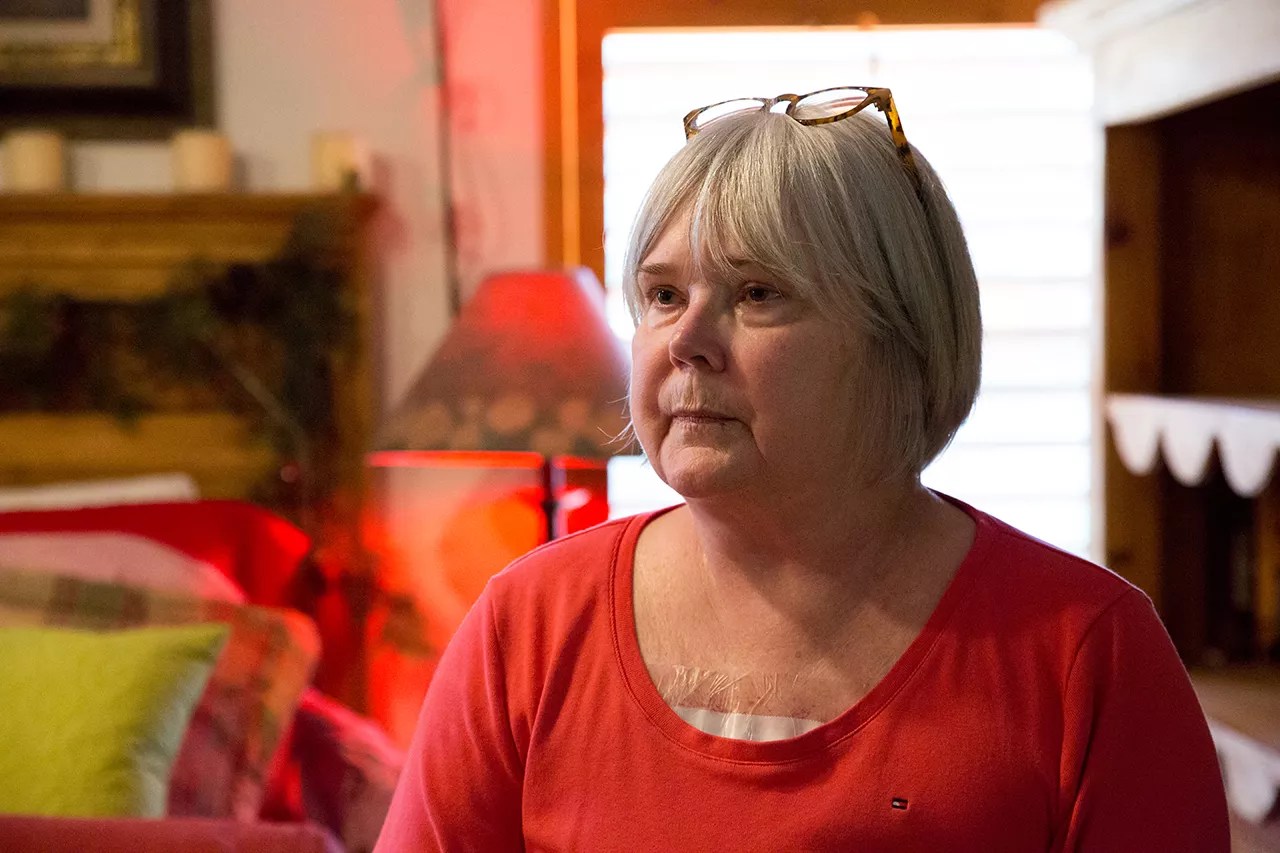
Danielle Lirette
Lee was born into a deeply religious family that spoke often about Hell. According to her, her family combined the Bible-thumping with physical, emotional and sexual abuse.
Lee, who was shy and struggled with a learning disability, didn’t make many friends as a teen at Arvada High School. But she surmounted those problems to graduate in 1965, and went on to earn both an undergraduate degree in history and a master’s degree in women’s history from Colorado State University.
She got married in 1968, to a man a few years older. They had a son and a daughter together and raised them in Loveland. Lee was mostly a homemaker while her children were growing up.
Her marriage was rocky and her husband emotionally abusive, she said. When they finally divorced, in 1994, the children, now adults, chose their father’s side. Lee’s relationship with them went from strained to nonexistent.
That same year, doctors told Lee that her ovaries needed to be removed because she was at risk of developing cancer. Following the surgery, she had her first manic episode and was diagnosed with bipolar disorder and, later, multiple personality disorder. She began experiencing hallucinations and delusions and was hospitalized at a behavioral-health center in Fort Collins.
Lee was diagnosed with breast cancer in December 1999 and underwent a double mastectomy. The surgery brought up latent trauma that, combined with the chemotherapy, contributed to her spiral into severe depression. Feeling suicidal, in 2000 she re-entered the Fort Collins facility.
Eventually, Lee found a career as an interior designer and built a business designing the insides of multimillion-dollar homes. She also wrote numerous memoirs.
She tried to lead a happy life, but the cancer persisted. She’d enjoyed years of good health before the cancer spread to her bones and chest wall in 2013. Treatment helped, but only for a few years.
In August 2018, the cancer in her chest wall returned. Her doctors told her she’d need surgery to fight it.
But Lee was done fighting a losing battle: “Even with this very unusual surgery that they were considering, it still wouldn’t get the cancer. After enduring the surgery, I would still be facing a cancer death sometime imminently.
“That point is when I finally realized that my body just couldn’t take it anymore,” she said. “I had always felt that needless suffering was sadistic and wrong and should be avoided at all costs.”

Danielle Lirette
In 1997, Oregon became the first state to legalize medical aid in dying, which gives terminally ill patients access to medication to end their lives at the time and place of their choosing. Efforts to pass similar legislation in Colorado began in 2015, when Representative Lois Court and Senator Joann Ginal introduced legislation that would have legalized medical aid in dying.
Denver attorney Julie Selsberg was a key driver in pushing the bill, testifying in favor of it at multiple hearings at the Capitol. After her father, Charles, was diagnosed with ALS in October 2013, he began researching medical aid in dying.
“At first it made me uncomfortable,” Selsberg says. “Then, as I read more about it and talked to him about it and watched him in his decline, I saw why this option exists and why it’s important for this option to exist.”
Charles thought about moving to Oregon, but he didn’t think he could fulfill the law’s residency requirement quickly enough. Just before dying in March 2014, he penned a letter to the editor of the Denver Post.
“Dear representatives and senators of the Colorado General Assembly,” it began. “There is no bill on this issue in this legislative session, but I’m hoping my statements will encourage you to consider one, if not this year, then soon. I have to give my testimony to you now, because by next week I hope to be dead.”
Selsberg and other advocates started presenting state lawmakers with examples of patients like her father to make the case for a medical-aid-in-dying law, but legislative efforts failed in 2015 and 2016. The strongest opponents were pro-life Christians, who argued that it was criminal to purposefully end a life.
The Archdiocese of Denver, for example, refers to medical aid in dying as suicide. “Suicide contradicts our natural inclination to preserve and perpetuate our life, and it also contradicts the way Jesus Christ accepted death,” according to the organization’s website.
But proponents of medical aid in dying argue that the religious beliefs of a few shouldn’t affect society as a whole. “If somebody has a deeply held religious belief that it is wrong to end your life before it’s God’s decision to do so, I can’t argue with that,” Selsberg says. “I just didn’t like that people who held that belief were telling others what to do.”
After legislative efforts failed, she and other advocates took the issue to the people of Colorado through a ballot initiative in November 2016; it passed with 65 percent of the vote. Similar laws exist in California, the District of Columbia, Hawaii, New Jersey, Oregon, Vermont and Washington state.
Colorado’s law gives a terminally ill person with six months or less to live the opportunity to procure and self-administer aid-in-dying medication, which comes in different forms. Doctors in states with older medical-aid-in-dying laws initially prescribed pentobarbital, a barbiturate often used for executions in the United States.
Secobarbital, another barbiturate, eventually became the drug of choice but has become too expensive for some patients. Most prescriptions are now written for a morphine compound that includes Valium and other medications that slow the heart. The medications generally put a patient to sleep quickly before stopping their breathing. Since the morphine compound also has medications that act on the heart, that organ sometimes stops first. Lee got her morphine compound for around $500 and paid out of pocket, since Medicare doesn’t cover end-of-life medication.
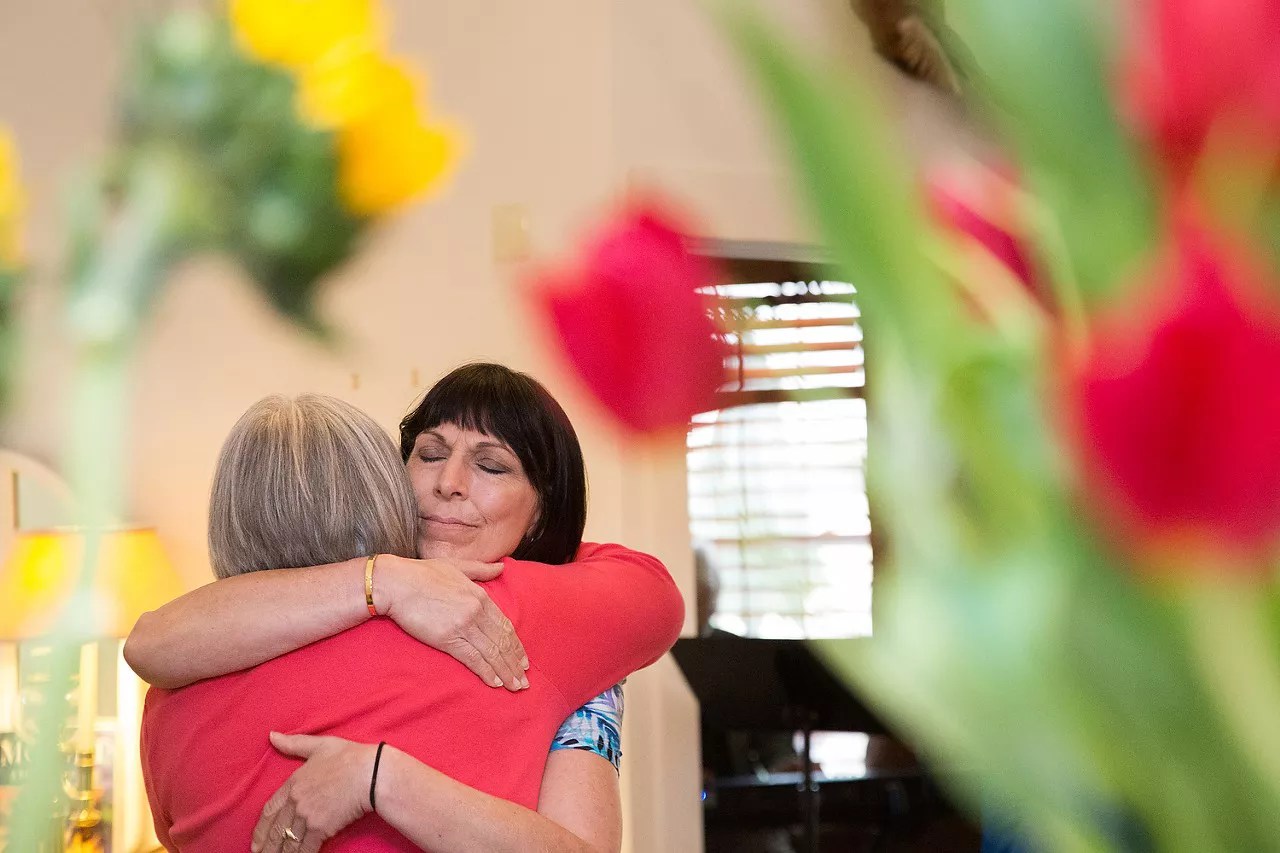
Lee and her friends hugged just before she went into her bedroom and took the end-of-life medication.
Danielle Lirette
The law created criminal penalties for tampering with an aid-in-dying request or coercing someone who is terminally ill to ask for the medication. Eligible candidates must be eighteen years or older and deemed mentally competent by their physician.
More than 200 people in Colorado have made use of the law. In 2017, 72 people were prescribed aid-in-dying medication; in 2018, that number jumped to 125. In 2018, 66 physicians in the state wrote prescriptions for the medicine. The majority of prescriptions in 2017 and 2018 were for the morphine compound, along with medication to ease anxiety and combat the physical effects of the aid-in-dying formula, such as nausea.
Most prescriptions have been for people like Lee who suffer from terminal cancer, but people with progressive neurological disorders, ALS and other ailments have also gotten them. Because a patient has to be deemed mentally competent and able to self-administer the medication, people with severe Alzheimer’s and other forms of dementia or those who can’t move their limbs don’t qualify.
In 2017 and 2018, slightly more men were prescribed end-of-life medication than women; most were older than 65. About two-thirds were from the Denver metro area, and most people chose to die at home, while a minority died in nursing homes.
Lee was the perfect candidate for end-of-life medication. She qualified in every regard and came to the conclusion of her own volition. But the law requires that two physicians sign off on a request for the prescription, a step that Lee found difficult to navigate.
The first physician she approached rejected her. “She spoke about having taken the oath to do no harm,” Lee said. “But what I realized was, she hadn’t even considered what it means to do no harm. Preventing somebody from horrific pain that can’t be stopped, from my point of view, would be to do no harm.”
Proponents of medical aid in dying say Lee’s experience is the rule, not the exception.
“A lot of it is confusing. It’s a lot to consider. It’s a lot to do. Finding a second doctor, it’s hard for somebody,” says Sam DeWitt, the Rocky Mountain West campaign manager for Compassion and Choices, an organization that helped push medical aid in dying in Colorado.
After the first rejection, Lee began working with UCHealth on finding physicians who would help her along her journey. Although some hospitals still don’t recognize the medical aid-in-dying law, the UCHealth system allows its physicians to sign off on such requests and its pharmacies to fill prescriptions for end-of-life medication.
Lee found two UCHealth physicians who would help, one of whom was a radiologist at a branch in Fort Collins. Recalled Lee: “She said to me, ‘Diana, this law is so good. I have seen so many women suffer, and they shouldn’t have suffered.'” (Lee’s physicians declined to comment for this story.)
The law is still controversial among physicians. The Colorado Medical Society, an organization that comprises doctors across the state, has taken a neutral stance on it. A February 2016 survey of its members, the most recent available, showed slightly over half supported it. In the same survey, 62 percent of Denver physicians supported it, while only about 49 percent of doctors from smaller cities backed it.
The American Medical Association, the largest body of physicians in the country, also opposes medical aid in dying, which it characterizes as “physician-assisted suicide.”
“It is understandable, though tragic, that some patients in extreme duress – such as those suffering from a terminal, painful, debilitating illness – may come to decide that death is preferable to life,” a statement from the AMA reads. “However, permitting physicians to engage in assisted suicide would ultimately cause more harm than good. Physician-assisted suicide is fundamentally incompatible with the physician’s role as healer, would be difficult or impossible to control, and would pose serious societal risks.”

Danielle Lirette
Opponents in the medical community often cite certain religious beliefs in their arguments. For example, Centura Health, one of the largest hospital chains in Colorado, doesn’t facilitate medical aid in dying. “Centura Health has a long tradition of believing in the sanctity of life, extending compassionate care and relieving suffering,” according to a statement from the hospital. “These fundamental values are reflected in the depth and breadth of support and comfort services we offer, including palliative care, hospice care, spiritual care services and mental health services, so patients and their families may live with dignity until the patient’s time of death.
Centura Health facilities and providers do not provide medical aid in dying medication or related services.”
Compassion and Choices’ DeWitt says he doesn’t try to dissuade opponents who cite Christian fundamentals. “We’re focused on secular institutions right now,” he says. “We’re trying to move the ball where there’s a ball to be moved. I don’t think there’s a ball to be moved with the religious institutions.”
Opponents worry about possible abuse of the law or coercion of terminally ill individuals. The Colorado Department of Public Health and Environment, for its part, says that it has never come across an instance of abuse or manipulation of the law.
“There’s years and years of data that demonstrate that this is a safe option, that vulnerable populations are protected from coercion. There’s never been a demonstrated case in the United States of that happening,” says Peg Sandeen, executive director of Death With Dignity, an Oregon-based organization that educates patients and doctors about medical aid in dying.
Sandeen points to the challenges that Lee encountered as examples of how people are actually protected from abuse. “The way the law is built is there’s a tension, there’s a deliberate tension between creating access and having safeguards that prevent against coercion,” she says. “All the hoops that a patient has to jump through are meant to make sure that someone in a vulnerable position can’t use the law.”

Lee will be cremated with some of her favorite mementos, and her ashes will be spread in Maui.
Danielle Lirette
As April 28 approached, Lee began crossing off items on her bucket list. She visited the Grand Canyon and dined with friends at some of her favorite restaurants.
She also started preparing for her final day. At first she expected that just a few people would show up to her end-of-life ceremony. But as she started telling people about her plans, it became clear that they wanted to be there to say goodbye.
“What surprised me was that once my friends heard what was going on, they have basically helped me turn it into a party,” she said. “I’ve really wanted people to understand that there is a good side to this right-to-die law in many, many ways.”

The end-of-life ceremony turned into a party after friends heard about Lee
Danielle Lirette
Lee chose April 28 because that’s when her friend Mike, a musician, was available to play.
Soon after the celebration began, around 10 a.m., it became clear that no one had ever been to a gathering quite like Lee’s. Usual party small talk was replaced with conversations about death, religion and the afterlife. A Christian and an atheist discussed what happens after death.
A friend spoke for Lee, saying she was neither someone who claimed to know what happens in the afterlife nor someone who felt sure that nothing comes after death. Others mentioned loved ones they had lost who suffered and might have opted for medical aid in dying if it had been legal.
Lee’s spirits were high as people from all aspects of her life came to say goodbye. A local police officer stopped by to give her one last hug. Her hair stylist also came, as did her CPA, her therapist, a friend from her time as a student at CSU, and two former professors. There were fellow interior designers, people she had met in dance classes, and women she’d met when she moved to Loveland.
Around 1 p.m., Lee gathered everyone in her kitchen to talk about things she was putting into a wicker box that would be cremated with her. She included a photo of some of her grandson’s artwork, pictures with friends and tiny shoes from her childhood.
Lee also spoke about how certain guests had influenced her. She felt a special connection to one guest in particular – the stepdaughter of her hair stylist – so she gave the teenager the keys and title to her SUV. Lee just had one request: that the girl put a picture of her under the driver’s seat so she could always be with her.

Lyrics from the song
Danielle Lirette
Following the box ceremony, Lee cut her cake, which had “I Did It My Way” – lyrics from the song made famous by Frank Sinatra – written on it. She had already given away her silverware, so guests ate with plastic forks.
Shortly after cake, a hospice nurse arrived. She gave Lee some anti-nausea medication to stave off any side effects of the aid-in-dying concoction and found a red goblet, from which Lee would take her last sip.
Around 3, Lee’s friends sang “Happy Trails,” the theme song from The Roy Rogers Show. Mike accompanied on the guitar.
Some trails are happy ones,
Others are blue.
It’s the way you ride the trail that counts,
Here’s a happy one for you.
Happy trails to you,
Until we meet again.
Happy trails to you,
Keep smiling until then.
Who cares about the clouds when we’re together?
Just sing a song, and bring the sunny weather.
Happy trails to you,
Until we meet again.
Lee then recorded her obituary on someone’s phone. Around 3:30, after she and her friends shared their last hugs, Lee went into her bedroom with the nurse and a close friend by her side. Out of sight from everyone, Lee drank the bitter medication, which she chased down with some honey that her friend had brought from her beehive.
Lee fell asleep before slipping into a coma, a process that usually takes about five minutes; death typically follows an hour to an hour and a half later. Lee was right on schedule: At 4:48 p.m., the 71-year-old was pronounced dead.
Lee had asked that her ashes be spread in Maui, one of her favorite places in the world. All of the proceeds from the sale of her home and her remaining belongings will go to St. Jude Children’s Research Hospital.
Just before taking the medication, Lee wanted everyone to know one important thing.
“Nobody tells us that planning your own death can be fun,” she said. “That’s the biggest-kept secret. But it actually is true. It’s true.”