
City of Denver

Audio By Carbonatix
Keep Westword Free
We’re $2,500 away from our spring campaign goal!
We’re aiming to raise $20,000 by April 26. Your support ensures Westword can continue watching out for you and our community. No paywall. Always accessible. Daily online and weekly in print.
Like so many cities across the country, Denver is suffering from an opioid crisis, with the number of individuals in the city using heroin and other opiates, and sometimes dying as a result, reaching new and increasingly worrisome levels.
The recently issued Denver Opioid Strategic Response Plan is an attempt to stem the epidemic, and Lisa Raville, executive director of the Harm Reduction Action Center, who participated in the report, sees it as a step toward helping those with addictions rather than demeaning them.
“I appreciate that there was a common thread about stigma and how that’s harming folks,” Raville says of the document. “The plan goes through the spectrum of prevention, harm reduction and treatment, and those subjects are so large that chipping away at them will take a lot of time. But I’m pleased that there’s the intention to reduce the stigma for drug users in our community.”
According to Raville, meetings related to the plan got under way “last September or October, and they did a really good job of getting a lot of stakeholders to the table multiple times: City of Denver agencies, mental health providers, myself, the library, the district attorney’s office, law enforcement. The first couple of meetings were kind of state-of-the-city – figuring out where we’re at and where we’re trying to go. And they they started firming it up.”
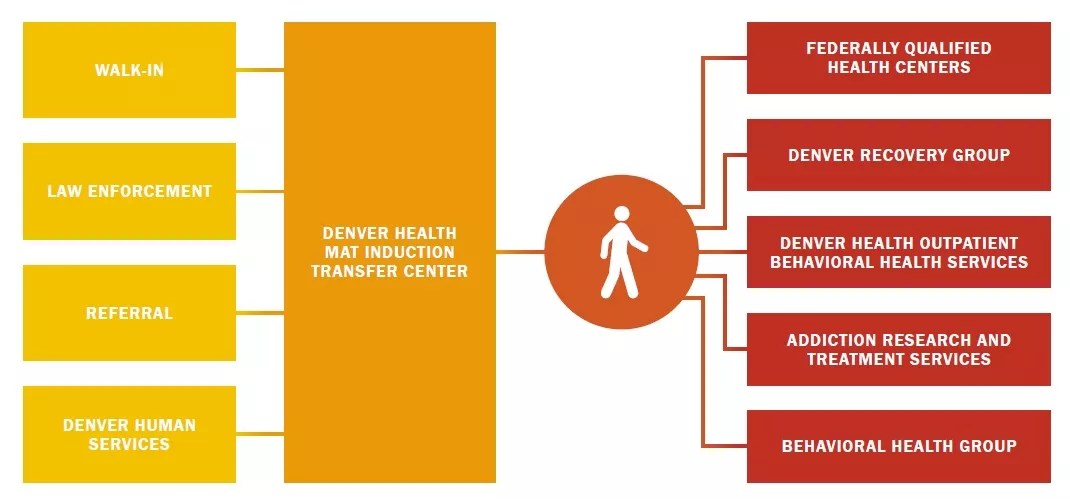
A graphic showing resources available to individuals with opioid addiction included in the Denver Opioid Response Strategic Plan.
City of Denver
The completed plan identifies three primary goals: “Prevent Substance (Mis)use,” “Improve Treatment Access and Retention” and “Reduce Harm.” Under these headings are multiple strategies for achieving the assorted targets, as seen in the following excerpts:
PREVENT SUBSTANCE (MIS)USE
STRATEGY A: Enhance capacity for effective prevention programming
STRATEGY B: Promote medication safety
STRATEGY C: Provide peer recovery support services• Increase the number of providers delivering evidence-based programs on adverse childhood events and trauma
• Increase the percentage of youth who report having a parent or adult they can talk to or go to for help
• Reduce the percentage of people who self-report experiencing stigma within the past month
• Reduce the percentage of people who report misusing substances in past year/past 30 days
• Reduce the percentage of patients receiving opioids in emergency departments
• Reduce the number of patients receiving overlapping opioid prescriptions
• Reduce the number of patients with overlapping opioid & benzodiazepine prescriptions
• Increase the number of agencies/providers that provide peer recovery servicesIMPROVE TREATMENT ACCESS AND RETENTION
STRATEGY A: Increase participation/enrollment of people with substance use disorders (SUD) in treatment services
STRATEGY B: Increase retention of people with substance use disorders in treatment services• Increase the number of people enrolled in treatment for SUD
• Increase the number of people seeking SUD treatment enrolled within 24 hours
• Decrease the number of repeat treatment admissions over calendar yearREDUCE HARM
STRATEGY A: Reduce rate of overdose deaths
STRATEGY B: Improve health outcomes among people who use drugs
STRATEGY C: Implement innovative service facilities• Increase the number of sharps collected at public kiosks
• Decrease the number of improperly discarded sharps in the community
• Decrease the number of fatal overdoses
• Decrease the number of nonfatal overdoses
• Decrease the number of new HIV cases attributable to drug use
• Decrease the number of HCV cases
• Increase the number of people who use substances who are retained in health care
• Increase the number of people utilizing innovative facilities
• Increase the number of facilities offering new or innovative services
• Reduce the number of emergency department visits and hospital discharges related to substance use
Some of the action items represent “things the city is already doing,” Raville acknowledges. “And you always want to have a prevention element. But I was especially appreciative that there was a lot of support for harm reduction in general. Harm reduction is definitely becoming a priority, and I think now cities and states across the country are starting to realize that they need to be working with people today for a healthier and safer them.”

A photo depicting a display of prescription bottles included in the Denver Opioid Response Strategic Plan.
City of Denver
An example involves the importance of ID cards for people struggling with addiction.
To get methadone and Suboxone, a pair of substance-use treatment options, at clinics, “you need to have some sort of an ID with a picture on it,” Raville explains. “But for folks who are homeless, often their stuff is lost or stolen or thrown away when they’re incarcerated. As a result, they often have a difficult time accessing treatment, especially since you need to get your birth certificate and a Social Security number to get an ID.”
The emergency department at Denver Health has established a pilot program addressing this situation – and Raville notes that staffers from the St. Francis Center visit the Harm Reduction Action Center weekly “to order birth certificates and social security numbers. And people can use our address as their ID address.”
Talking about such challenges with members of law enforcement was important, Raville believes. “I’ve heard them say, ‘I don’t understand why these people can’t be in treatment.’ So I appreciated having those conversations, so we could explain how things really work. Harm reduction and treatment have been very siloed in our community, so this was working together in a way we haven’t always been able to do before.”
Another element of the plan that cheers Raville is a section in which “we were able to reduce the barriers to opening a supervised consumption site in Denver.”

Lisa Raville at the Harm Reduction Action Center.
Photo by Michael Roberts
Last year, a group of legislators and others taking on the opioid issue approved a pilot program for such a facility, also known as a safe-injection site – but a bill that would have authorized it was killed in the general assembly during the 2018 session. For such a site to move forward, she says, “we need to have ordinance changes and legislation. So I take that section as, ‘Let’s remove the barriers – challenge accepted.’ I’m hoping to have a city ordinance change and state legislation in 2019.”
Another positive from Raville’s perspective involves testing strips for Fentanyl, a powerful synthetic opiate whose addition to heroin can have lethal consequences. “We now have testing strips for folks, so they can test their drugs to make sure there’s no Fentanyl in there,” she reveals. “I’m really pumped about that, because it should help reduce overdose deaths. And I’m also very supportive of having more public syringe disposal kiosks. There are only three 24-7 kiosks in the city, and we need more. If people want to dispose of a syringe properly, it’s hard to do right now. We need to make it easier.”
While a lot of the attention related to opioids nationally has involved prescription medication abuse, Raville was pleased that the plan doesn’t shrug off those using street drugs. “When you’re talking about Colorado and Denver, you’re talking about black tar heroin, and that means people are injecting it,” she emphasizes. “So we definitely made sure throughout the process that these folks’ voices were prioritized. A lot of people are struggling. Many heroin injectors are homeless or transitionally housed, and it’s difficult to ask homeless folks to be sober. So I and a few others talked about these challenges and how people who are injecting in our community deserve the same respect as any other drug user.”
The plan arrives at a time when other resources for opioid users are vanishing. “Arapahoe House closed in January,” Raville allows, “and the Salvation Army’s in-patient facility is closing September 1. They served marginalized folks. That’s one reason why treatment on demand is so essential for the people we serve.”
Overall, though, Raville is upbeat about having “a good plan that’s very action-oriented. And we’re on the case.”
Click to read the Denver Opioid Response Strategic Plan.